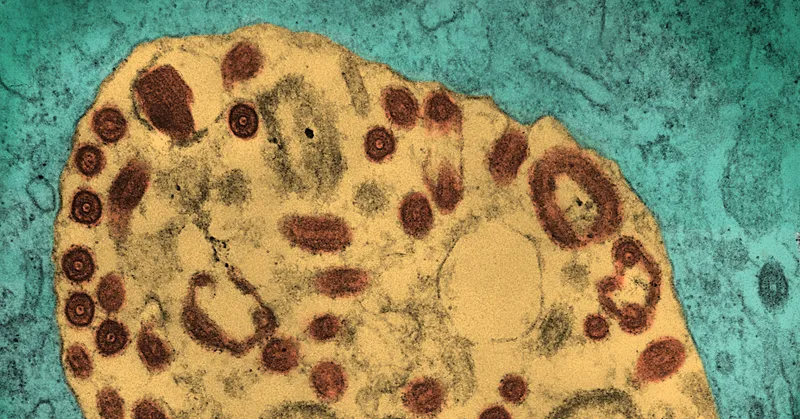
If a virus like Marburg is spreading, being able to do genetic sequencing locally is particularly useful to find a way of reining it in. Genetic sequencing helps researchers keep track of any changes to the virus, and how these could affect patients.
But in countries like Tanzania and Equatorial Guinea, sequencing capacity is limited. The risk of decimation of populations is ever so higher.
“Without knowing the variants, and subsequently how the virus is evolving, knowing the impact on health and severity will remain a challenge,” says Mohamed Zahir Alimohamed, a human genetics scientist at Tanzania’s Muhimbili University of Health and Allied Sciences.
When the fisherman’s relatives fell ill, they were admitted to the Maruku Health Centre in Bukoba. A lab technician who handled their samples caught the virus and died. And of the three surviving patients, one is a health worker.
This suggests the local health services didn’t have sufficient protocols in place for dealing with potentially dangerous pathogens, which is something countries across the continent must improve, says Loveness Isojick, an infection prevention and control nurse activity manager at Médecins Sans Frontières. “There is a need to be proactive, and to have [viral haemorrhagic fever] contingency plans,” she says.
This, Isojick argues, needs to go beyond the basics of just infection control. “We need to look into ways of managing special cases, like pregnant women. What about the discharge package for the males who were positive, so that they do not infect their spouses after recovery?” she says. Marburg virus has been documented in the semen of male patients up to seven weeks after they have recovered.
To date, no additional cases have been detected in Tanzania, and the outbreak hasn’t reached beyond Bukoba. One of the three patients receiving treatment has been discharged. The virus appears to be under control there. But in Equatorial Guinea, infections and deaths haven’t been contained. This can also be traced back to insufficient laboratory testing capabilities in the country.
Early on in the outbreak, samples from suspected patients had to be taken to neighbouring Gabon and Senegal for processing. Since then, reported confirmed cases have risen from one to 13, with nine patients dying. At least 20 probable cases – all resulting in death – have also been identified, and on top of this, the WHO has said that there are additional lab-confirmed cases in the country – but that these haven’t yet been officially reported.
Worryingly, the confirmed cases are spread across three provinces, some 150 kilometres apart, suggesting viral transmission is happening undetected. The Ministry of Health has launched a public health emergency operation to contain the outbreak – but with better testing capacity early on, this might have happened much quicker.
It’s not just Marburg’s high fatality rate that makes it a grave concern, says Tanimola Akande, professor of public health at the University of Ilorin in Nigeria. “It has the potential to spread across borders.” Cases have been identified in Europe and the United States in the past, when tourists returned from holidays in East Africa.
Indeed, the virus gets its name from the German city of Marburg, following an outbreak there in 1967 that contributed to its identification (although that outbreak originated from imported African green monkeys, not humans).
A big unanswered question is whether the current outbreaks in Tanzania and Equatorial Guinea are linked – the public health agency for the continent, the Africa Centres for Disease Control and Prevention, is running sequencing to find out.
If the outbreaks are related, they illustrate how a future spillover event could easily cascade into a global outbreak if a pathogen isn’t contained and infected people travel overseas.
For now, in Tanzania, 205 people who may have had contact with the infected have been put under close monitoring.
Meanwhile, health authorities are promoting measures in Bukoba to keep the virus from spreading (such as hand washing and social distancing), ensuring that any burials in the area are safe and highly supervised, and monitoring travellers leaving the wider region for symptoms.
“We are scaling up awareness campaigns,” Mwalimu, the Tanzanian health minister, said during a press briefing.
In Equatorial Guinea, the full scale of the outbreak has yet to reveal itself – government reporting of cases has been slow, and the geographical spread of those logged so far suggests there’s been unreported transmission.
To get on top of the virus, the government has the Emergency Response Plan for Marburg Virus Disease, developed with the WHO and Unicef. But this is a very limited set of actions – essentially the same as those being used in Tanzania: monitoring contacts of the infected and spreading the word about good hygiene practices.
There are at least candidate vaccines for Marburg – and they are being tested during this outbreak. But if the current Marburg outbreaks had been bigger, the several thousand experimental doses ready to deploy wouldn’t have been enough to conduct ring vaccination.
The virus is a known threat, but there aren’t abundant supplies of vaccines to test against it.
And what if the next pathogen to emerge is something that’s never been seen before, and there are no experimental vaccines available at all? If that happened, the world would be relying solely on quick testing and effective containment to stop the disease from spreading.
As the Covid-19 pandemic showed – and Marburg is now underlining in Equatorial Guinea – this is something countries still need to get much, much better at.
- A Wired report