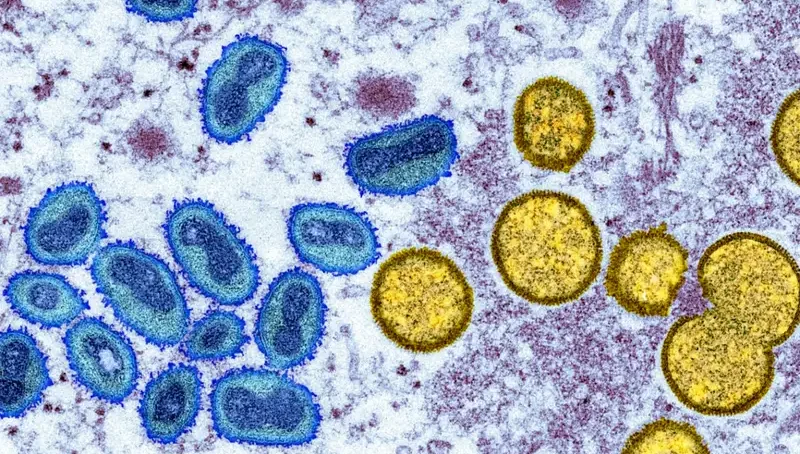
The number of reported monkeypox cases is rising rapidly in the largest known outbreak outside of Central and West Africa, where the virus is endemic.
At the time of writing, 172 confirmed cases have been recorded in North and South America, Australia, the Middle East, North Africa and across Europe, according to a list of reports compiled by Moritz Kraemer at the University of Oxford, John Brownstein at Boston Children’s Hospital in Massachusetts and their colleagues.
These same regions also have a total of 87 suspected cases of monkeypox and 27 people hospitalised with the infection. As of May 23, the UK had recorded 57 cases of the virus, and it appears to be one of the hardest-hit countries so far. No deaths have been reported anywhere in the world, according to the World Health Organization (WHO).
In the past, outbreaks outside of Africa have usually been linked with travel to endemic regions of the continent. A small 2021 outbreak in the UK occurred after someone travelled from Nigeria to Manchester. In 2003, monkeypox entered the US after exotic pets including mice and squirrels were imported from Ghana. These animals are thought to have transmitted the virus to humans.
The current outbreak is unusual in that infections seem to be mostly spreading between humans with no recent travel links to affected regions of Africa, suggesting the virus is being transmitted undetected in the community. This is the first time cases with no travel history have been reported in Europe, according to the European Centre for Disease Prevention and Control (ECDC).
Monkeypox is usually mild, with most cases resolving within a few weeks without treatment. Bulletins from organisations like the WHO, US Centers for Disease Control and Prevention (CDC) and the UK Health Security Agency (UKHSA) mean countries are actively looking for the infection, which has probably caused instances to be identified that would otherwise have slipped under the radar.
Nevertheless, monkeypox cases are expected to rise, at least in Europe, over the coming months. “As we enter the summer season in the European region, with mass gatherings, festivals and parties, I am concerned that transmission could accelerate, as the cases currently being detected are among those engaging in sexual activity, and the symptoms are unfamiliar to many,” the WHO’s regional director for Europe, Hans Kluge, said in a statement.
Early symptoms include fever, headache and muscle aches, sometimes followed by a chicken-pox-like rash that causes scabs.
Monkeypox isn’t considered a sexually transmitted infection, but can spread via skin-to-skin contact or sharing bedding with an infected person. In the UK, early cases were largely seen in gay men, bisexual men or men who have sex with men.
“We would recommend to anyone who is having changes in sex partners regularly, or having close contact with individuals that they don’t know, to come forward if they develop a rash,” Susan Hopkins, the UKHSA’s chief medical adviser, told the BBC.
In the UK, close contacts of those infected with monkeypox are being advised to isolate for 21 days by the UKHSA and are being offered a smallpox vaccine, which is 85 per cent effective at preventing a monkeypox infection. According to Politico, 1000 doses of the vaccine have already been administered in the UK, with just 3500 doses left.
Belgium has also mandated that those who test positive for monkeypox must isolate for 21 days. In the US, the CDC is advising people with monkeypox to isolate.
In Europe, the ECDC has urged countries to prepare infection-control strategies, such as increasing contract tracing and readying vaccines.
- A New Scientist report






